For many years pharmacy organisations such as the Pharmacy Guild and the Pharmaceutical Society of Australia have been proactive in seeking to expand the role that pharmacists play within the healthcare system. Pharmacists are highly trained professionals, experts in medication management, and are knowledgeable in disease management and prevention. With the current ongoing challenges being faced by the Australian healthcare system, due to an increasing ageing population, rising rates of chronic disease and general practitioner (GP) shortages, the various state governments have started looking for alternative solutions to the current crisis.
In September of this year, the Queensland government announced the Urinary Tract Infection Pilot program was to be made permanent, opening the way for other states and territories to consider similar programs. A subsequent pilot program, the North Queensland Community Pharmacy Scope of Practice Pilot was also announced in October of this year.
These announcements have been followed by each of the states and territories subsequently announcing their own intentions of increasing the scope of pharmacists practice to ease the current pressures on the health system. These programs include:
- Pharmacist prescribing for medications such as the oral contraceptive pill, antidepressants for patients on stable therapy, migraine, eczema, asthma, emphysema, nausea, vomiting and reflux medications.
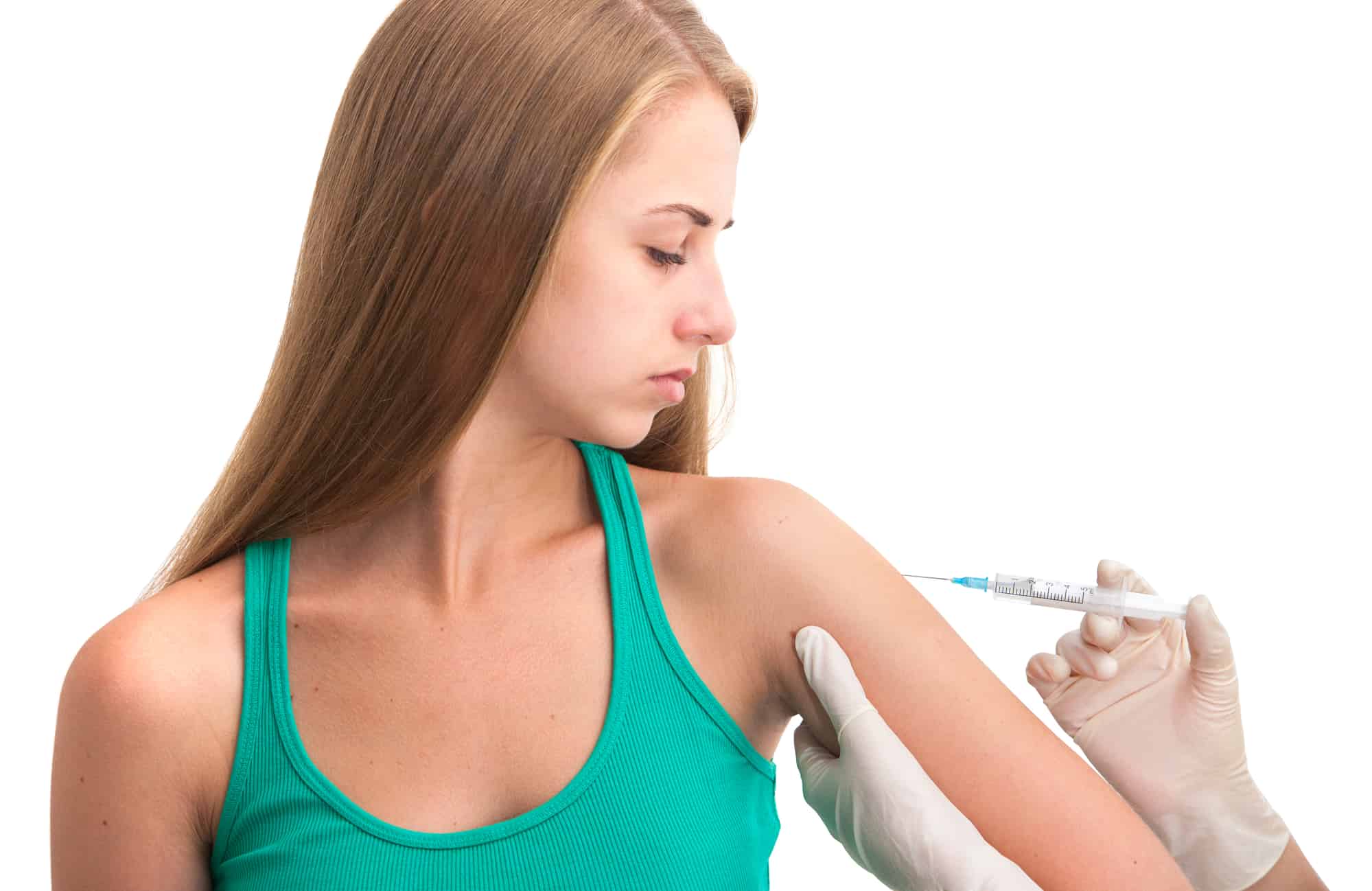
- Increasing the range of vaccines pharmacists provide eg. travel vaccines, shingles vaccines, and allowing administration of National Immunisation Program (NIP) vaccinations.
- Ability to treat minor ailments such as eczema, ear infections and uncomplicated urinary tract infections (UIT’s).
- Increasing the funding for a range of services such as oral health screening, weight management and smoking cessation.
Pharmacists who are able to work to their full scope of practice have an opportunity to not only fully contribute to the healthcare system but to increase the range and capacity of services available to a population. There are opportunities for pharmacists to improve medication compliance and increasing screening services to allow for early diagnosis and preventative care. This could lead to decreased waiting times and greater access to care, particularly in regional and remote communities. Access to pharmacists compared to GP’s in regional and remote areas are 1-3 or more times greater, compared to 2-3 or more times greater in metropolitan areas.
A report released by the Grattan Institute on 4 December 2022 called “A new Medicare: strengthening general practice” makes numerous recommendations including the suggestion that the federal government needs to “expand access by making general practice a team sport, with more clinicians using all their skills to share the load with GPs”. The report suggests the government should “fund 1,000 new nurses, physiotherapists, mental health clinicians, pharmacists, and other allied health workers in the highest-need communities, to work within general practices alongside GPs and provide fee-free care”.
GP Pharmacist John Woodward, has worked at a local medical practice in Pomona on the Sunshine Coast for 10 years. Due to the inability for the practice to find GP’s it is scheduled to close later this month. “This will have a devastating effect for the growing hinterland town and region with patients forced to seek care at other surrounding medical practices that are already at capacity”, he said.
During his time in the practice John has had a pivotal role in supporting the GP’s within the practice by providing patient education, answering medicine related queries from patient’s, GP’s and nurses, providing Home Medication Reviews (HMR’s), and providing formal eduction sessions to optimise medication prescribing habits.
“If the government were to provide funding for GP integrated pharmacists this would help alleviate some of the pressures that GP’s are currently facing on a day-to-day basis”, says John. “Many of these services could be performed using the current telehealth model, which is convenient and would increase access particularly in regional and remote areas”.
Pre-COVID, gaps in rural and remote health care were largely filled by overseas-trained graduates. However, border closures have meant those roles have been left unfilled. Besides the difficulty attracting new doctors, existing GPs are on the brink of burnout and are retiring earlier than expected. Unfortunately it is the patients who will suffer, potentially delaying care and adding further pressure to an already at capacity hospital system.
There has never been a more important time for pharmacists to step up and fully collaborate and deliver the highest standards of clinical care. In doing so we have an opportunity to alleviate some of the pressure on the healthcare system and assist in improving medicine management, access and the wellbeing of patients all across Australia.



 Share
Share